Working at the intersection of health and environmental sustainability
The Southeast Asia region is renowned for its cultural diversity and rapid economic growth. However, it faces a critical challenge that extends beyond national borders, namely, the intersection of health and environmental sustainability.
As the healthcare system across the region strives to meet the increasing demand for universal healthcare while aligning with the guidelines for climate resilience and sustainability in healthcare, the associated environmental impact has become a pressing concern.
The health sector constitutes a significant portion (10%) of the global economy and simultaneously contributes to environmental degradation by generating substantial waste and emitting pollutants, which account for 5.2% of global greenhouse gas emissions. Central to this challenge is the unsustainable procurement of non-medical and medical supplies, rampant consumption of single-use plastics, inadequate waste management practices, and the indiscriminate use of harmful chemicals within healthcare facilities contributing to 70% of emissions from the supply chain.
These practices in healthcare not only contribute to the region’s environmental degradation but also pose direct threats to public health, contributing to the triple planetary crisis. Recognizing the complex interplay between healthcare operations and environmental impact, there is an imperative to institute a comprehensive environmental sustainability program.
In addition, given the region's crucial priorities and building on the past and current work of Health Care Without Harm Southeast Asia on mercury and dioxins by mercury elimination and banning of medical incinerators, there is an urgent need to detoxify and decarbonize the healthcare system and establish sustainable measures to mitigate their impact through sustainable procurement, plastics, waste, and chemicals.
The Issue
The environmental sustainability conundrum within the Southeast Asian healthcare sector is multifaceted, encompassing unsustainable procurement practices, unbridled plastic consumption and use, inadequate waste and chemicals management.
The procurement of medical supplies often neglects sustainable sourcing and the absence of toxics-free criteria, leading to resource depletion and environmental impacts. During the COVID-19 pandemic, plastics, which are ubiquitous and omnipresent in the healthcare setting, contribute significantly to pollution. Improper waste management compounds these issues, increasing human health risks to the public. Additionally, the unchecked use of harmful chemicals from disinfectants and plastic products further exacerbates environmental degradation.
There is a need for a coordinated and intersectional approach to environmental sustainability programs tailored to the unique challenges of the health sector. To address this critical issue, the program should integrate sustainable procurement, detoxification of plastics, waste minimization, and sound management of chemicals, fostering a healthcare system in Southeast Asia that not only meets the health needs of people but also champions the well-being of the environment on which it relies.
Our Objectives
The program engages with the local and national government, healthcare facilities, health professionals, vulnerable populations, and regional multilateral bodies to achieve the following objectives:
Powerbuilding to influence regional initiatives on procurement, plastics, waste, and chemicals through policy advocacy and communications.
Improve procurement awareness and practices in health institutions, key countries, and agencies through advocacy, training, criteria adoption, and advanced market option.
Advocate, raise awareness, and mobilize networks for the reduction, detoxification, and decarbonization of products in the health sector in collaboration with regional strategic allies and partners.
Promote waste minimization and improve waste management while leveraging the issue to support Climate and GGHH and extend to the communities through advocacy, training and support for national initiatives.
Our Focus
Health systems wield considerable influence, both in the processes directly involved in delivering healthcare and in the broader spectrum of products they acquire and consume. A pivotal point of impact within healthcare delivery lies in the supply chain, in which procurement encompasses a diverse array of products, including chemicals, plastics, medical devices, and pharmaceuticals. A transformative call to action for mitigating these impacts lies in establishing and implementing sustainable and ethical procurement policies.
In 2019, Health Care Without Harm, through its SHiPP Project, piloted standards development and integration of sustainability criteria in procurement practices. This initiative aimed to drive market transformation and ensure that products used in the health sector have minimal negative impacts on human health and the environment. The development of the procurement standard with HCWH strategic partners in India, China, and Vietnam kickstarted a significant opportunity for sustainable products and capacity building among health systems, procurement officers, and suppliers. The SHiPP Project focuses on three areas: carbon reduction, safer chemicals, and sustainable resource use, and integrates criteria for sustainable products and implementation of sustainable procurement practices.
The healthcare industry’s use of plastic products poses a direct threat to human health. Many plastic healthcare items contain toxic chemicals that can be carcinogenic, mutagenic, reprotoxic, or endocrine-disrupting. Moreover, no consensus exists on these chemicals' safe or tolerable exposure levels. Therefore, adopting a precautionary approach to prevent exposure is imperative, particularly during critical stages of human development like fetuses, neonates, infants, and children. These groups are the most vulnerable and at high risk of experiencing adverse health effects due to exposure to plastics.
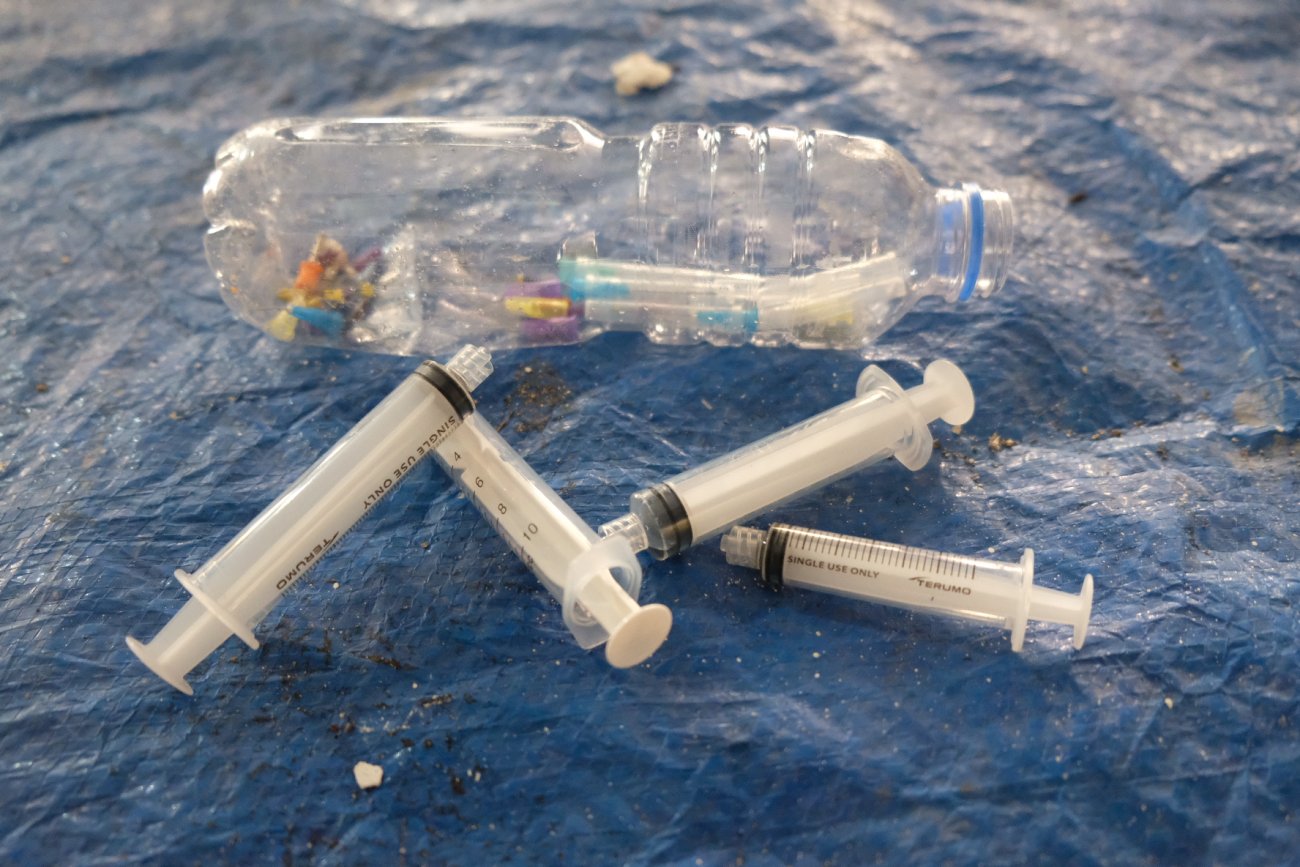
The use of plastic in healthcare has become ubiquitous and is found in almost every aspect of the industry. This includes single-use non-medical and medical devices. Shocking findings from waste audits conducted by Health Care Without Harm in healthcare facilities across the Philippines and Indonesia reveal that plastic comprises a staggering 46-72% of hospital waste. With most plastic items not being labeled, it becomes a challenge to make informed decisions for patients because the negative impact of plastic is felt throughout its life cycle. It is crucial to have policies that promote a circular economy that is just and transparent and based on necessary products, climate-smart, non-toxic, non-polluting, designed for reuse and long life, easy to recycle, and safe disposal options.
What started out in the Philippines as a global campaign to ban mercury in sphygmomanometers, and thermometers, the work has now expanded to chemicals of concern in medical devices as an issue that needs to be addressed to highlight “no exemption even in healthcare” in banning of single-use plastics. In a resounding call to action, HCWH SEA underscores the urgency of tackling the pervasive issue of plastic pollution through multiple spaces, including the Global Plastics Treaty. This includes the imperative of mandatory product labeling, a progressive reduction strategy for plastics, and a comprehensive approach to both intentional and unintentional plastic pollution. This recognition is particularly crucial in the wake of the COVID-19 pandemic, where the surge in plastic waste demands immediate and concerted efforts beyond the crisis, signaling a pivotal moment for sustainable healthcare practices.
Human activities, including the operations of healthcare facilities, generate waste. It has become increasingly evident during the COVID-19 pandemic that proper management of healthcare waste is imperative to prevent human health risks and environmental degradation. According to the WISH Policy Paper on Managing Healthcare Waste, which was led by HCWH, waste generation in hospitals in Southeast Asia ranges from less than one kilogram per hospital bed per day (kg/bed/day) to over eight kilograms per hospital bed per day. Of the waste generated, 15-25% is hazardous waste which can potentially transmit infectious diseases from sharps injury, exposure to staff and population, and leeching to air, land, and water.
Health Care Without Harm (HCWH) Southeast Asia (SEA) has undertaken multiple waste audits, with a specific focus on plastic waste, using specialized tools developed for this purpose. HCWH SEA strongly advocates for waste minimization and achieves this through advocacy campaigns, policy development, training, and stakeholder engagement. Waste management is a crucial yet often overlooked aspect of healthcare facility management. However, many healthcare facilities now recognize the significance of proper waste management to prevent occupational hazards and promote safety. HCWH SEA is at the forefront of promoting best practices in waste management across the region.
HCWH SEA has been actively involved in advocating for the ban of burn technologies and promoting safe and environmentally sustainable waste management alternatives. Recently, a bill on waste-to-energy was proposed in the Philippines, and in response, HCWH SEA developed a position statement calling for preventive and precautionary approaches, as well as prioritizing scientific evidence-based policy-making.